What Consumers Most Want from Health Insurers’ Technology
People don’t crave the latest fitness wearable. Their overwhelming preference is for simple applications that provide and organize information.
A version of this article appeared in the Winter 2016 issue of strategy+business.
In the $3 trillion United States healthcare industry, choice has swung decisively toward consumers in recent years. Empowered by technology, encouraged by employers, and incentivized by new regulations and products, more and more people are playing an active role in managing their own wellness, medication choices, and treatment options.
In response, incumbents and startups in the insurance industry are investing feverishly to roll out products and services that will appeal to consumers. Taking a cue from the technology and communications industries, many are pursuing disruptive technologies that promise to revolutionize the healthcare experience — whether they are digestive sensors or systems that allow doctors to examine and treat patients via video.
But here’s the thing: Consumers aren’t ready for a revolution. They have far simpler demands and desires, such as an easier way to schedule doctor visits or the ability to get follow-up notifications on a mobile phone. As a result, insurers that want to make the most of their investments in new technologies should focus their resources on developing simple digital products and services that align with their identities, strategic goals, and existing capabilities.
Consumers aren’t ready for a revolution. They have far simpler demands and desires.
This seemingly counterintuitive finding emerged from a recent survey by Strategy&, PwC's strategy consulting business. We asked more than 500 consumers to provide relative rankings of 15 technology-enabled features they wanted from their health plans. The results may be surprising (see Exhibit 1). The four most preferred features were all basic ones, such as out-of-pocket cost estimators and online appointment scheduling; meanwhile, futuristic solutions such as integrating wearables and interactive tools for self-diagnosis wound up in the “not as important” bucket.
It is true that the value of such advanced technologies lies in their ability to improve quality and reduce system cost. And as Steve Jobs famously put it, customers don’t always know what they want until it is shown to them. Nonetheless, respondents made it clear they want insurers to meet their basic needs before rolling out transformative features. Our analysis indicated that 94 percent of respondents chose features that offer basic utility and transparency over advanced or clinical-type offerings, such as telemedicine or in-home blood testing. Consumers also said they wanted more collaboration between payors and providers, and, surprisingly, said that they were open to receiving health and wellness advice from their insurers. In short, they’re worried more about the clock accurately telling time than about all its bells and whistles.
Keeping It Simple
The idea that customers prefer simplicity may not come as a shock to those outside the healthcare industry. But it’s likely a revelation to those in the business, especially the insurers that have been investing heavily in telemedicine and other advanced features.
The survey revealed further insights into consumers’ preference for simplicity and a streamlined experience. Some 97 percent of respondents said they would be willing to share personal health data and nonsensitive information if it would enhance their care, and only 3 percent ranked data privacy as the most important feature of a health plan. About half of consumers want to involve both providers and insurers in their healthcare, and consumers are becoming increasingly comfortable with receiving wellness advice from health plans. That makes sense given the growth of so-called consumer-directed health plans, which put more responsibility for healthcare decisions and costs on consumers. Patients are also routinely receiving health advice and care from other nontraditional sources. For example, a growing number of U.S. residents get their flu shots at CVS or their annual physical at Walmart.
In expressing their preference for user-friendly interfaces and convenience, consumers are drawing on their experience with technology in such industries as banking and retail. These industries have deployed digital technology to eliminate much of the friction of everyday transactions. With a few swipes and keystrokes, consumers can book haircut appointments online; compare airfares; and read and share user reviews of restaurants, hotels, and plumbers. Even more complex tasks — doing taxes, trading stocks, or filing insurance claims — can now be performed on a smartphone. The yawning convenience gap between the user experience in other industries and the user experience in healthcare has led consumers to seek greater technological assistance from their health insurers.
The lesson for incumbent health plans is to stick with enhancing convenience and resist the temptation to jump into territory that technologically advanced competitors and industries such as banking and retail are now exploring. Those companies are pushing ahead only because they have already mastered the basics. Our survey shows that health consumers don’t expect the industry to make that ambitious high-tech leap — and that they don’t want it to. The results imply an awareness that healthcare lags other industries in its adoption of consumer technology.
Indeed, insurers would be well advised to look at the example set by the banking sector to see how staging a gradual evolution of improving basic consumer experience and eliminating frustration can be preferable to rushing headlong into a set of futuristic technologies. Throughout the early to mid-2000s, online banking didn’t fully catch on: The technology wasn’t ready, the cost savings weren’t substantial enough, and too few customers saw the value or utility of transacting business online. It was only after customers grew comfortable with the foundation of a simple portal that the banking industry began to roll out advanced technologies that aligned with consumer demand, such as mobile check deposits.
In order to win consumer engagement, trust, and loyalty, payors need to invest in developing basic capabilities focused on cost, transparency, and convenience that streamline the healthcare experience. These investments will be substantial, but payors that fail to deliver on the basics risk leaving significant value on the table. Our project experience shows that investing smartly in the right technology can yield an 8 to 12 percent positive impact on operating margin via increased revenue, improved behavior and medical outcomes, and reduced bottom-line cost.
The best example today of a payor delivering the basic features consumers want might be Oscar Health, a health insurance startup based in New York. In a few short years, Oscar has amassed 125,000 members in four states by providing coverage through a mobile app that packs all aspects of consumers’ health management into their smartphones. Oscar offers sophisticated features such as telemedicine. But its attraction for consumers is the “simple and easy” mantra on which it prides itself. Oscar provides basic cost-comparison details that facilitate a one-click enrollment process, so users can take less than five minutes to become a member. It is convenient and transparent.
Picking a Way to Play
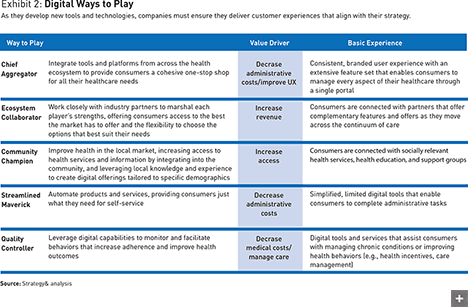
Of course, not every payor has the luxury of starting with a clean slate. Established insurers need to figure out how to deliver on existing promises while creating customer experiences that are unique to their brand and aligned with their strategic outlook. In other words, the path insurers choose going forward should depend in part on the path they’re already on. We’ve created a framework that helps insurers develop the right capabilities and decide where to invest on the basis of who they identify as their core customers, and the value they want to deliver (see Exhibit 2). Each of the five ways to play we’ve identified is based on a payor’s strategic imperatives and existing capabilities, and results in a different consumer experience.
Chief aggregators, like Amazon in the retail industry, integrate a range of tools and platforms to provide one-stop shopping, and need to provide branded user experiences that offer comprehensive features through a single portal.
Ecosystem collaborators, such as Visa in financial services, work with industry partners to offer flexibility and choice, developing services that offer relevant features and information as customers move through the continuum of care. A community champion, such as the YMCA in the physical fitness arena, focuses on improving health in the local market and connecting consumers with demographically relevant services and information. Streamlined mavericks, such as Walmart in retail, automate the process for self-servicing customers, building simple tools that let consumers complete administrative tasks. And quality controllers, such as FedEx in logistics, monitor and facilitate behaviors, and develop easy-to-use interactive tools aimed at managing chronic conditions or encouraging specific outcomes.
No insurer will fit neatly into just one of these categories. But choosing a dominant model can help insurers develop a strategic framework to guide investment decisions. Our research has shown that most companies direct 20 to 40 percent of their technology budgets toward investments that have nothing to do with their overall strategies. And in the current climate, insurers simply cannot afford such waste. An insurer that wants to be a chief aggregator, for instance, should direct investments toward capabilities that bring together in one place functionalities such as finding providers, scheduling appointments, and estimating costs. An ecosystem collaborator might not emphasize its investment in an integrated platform, but would spend heavily on building partnerships to provide an expansive ecosystem of features.
Although payors should direct the bulk of their investments toward technology that aligns with their strategic priorities, they shouldn’t ignore other basic tools such as cost estimators and payment mechanisms. Our health consumer survey makes it clear that consumers want all payors to provide those essential applications. And all payors should be integrating their data sets with providers'. The state of affairs in which hospitals possess consumers' health records (charts, doctors’ notes, test results) while insurers have all their billing information isn’t tenable. Payors should build interfaces that allow consumers to view and manage every aspect of their healthcare through a single portal.
Health plans are certainly right to push for greater innovation. Failing to do so in today’s fast-paced new health economy spells an almost certain death by disruption. But as in any other business, fixating on the horizon can mean missing immediate opportunities to give consumers what they actually want. It may mean skipping a vital first step on the ladder to long-term viability. Providing customers with tools and services that meet their basic needs is crucial if companies are to win trust. And in an area as sensitive as health, consumers will come along on the journey to unfamiliar methods of delivery only if they trust their counterparts. The first step in preparing for a more complex future may be to focus on keeping things simple in the present.
Reprint No. 16401
Author profiles:
- Keith Fengler advises executives on consumer-driven strategies and digital health innovation for Strategy&, PwC’s strategy consulting business. He is a Boston-based principal with PwC US.
- Jaime Estupiñán is a thought leader in consumer-capable health for Strategy&. He is a New York–based principal with PwC US.
- Kenny Chan is a thought leader in digital health who focuses on consumer experience. He is a Boston-based director with PwC US.
- Also contributing to this article were PwC US principal Jay Godla, senior associate Nina Vishwanath, and associate David Zhang.