Health Care’s Retail Solution
A robust retail market is emerging from the ashes of the current health-care system.
 |
|
Illustration by eboy
|
Imagine a future in which the health-care system provides consumers high-quality care in a variety of convenient forms at competitive prices. In this vision, insurers, employers, and governments offer consumers financial incentives to take better care of themselves — to exercise, eat right, stop smoking, and follow treatment regimens for chronic problems such as asthma and diabetes. The system encourages consumers to plan for the health-care needs they can anticipate (i.e., nonemergencies) by “shopping” for products and services much as they do for a new car; consumers make informed decisions based on readily available reports on quality, service, and price. Providers and product manufacturers compete for different segments of the market using a variety of channels, formats, and business models. And consumers confused by the profusion of offerings can turn to agents who help them design the most suitable health-care programs for themselves and their families.
Such a robust retail health-care market is more than a vision; it is a real possibility. Today’s troubled U.S. health-care industry is the result of decades of good intentions and unintended consequences. Payers (defined as government and employers, who foot the bill for most health-care costs) and patients alike struggle to cope with complexity and cost. But most efforts to control costs — by government and by the private sector — have proven unsustainable and have unintentionally increased complexity. The upshot is a situation in which only 61 percent of employers offer coverage for active employees, approximately 30 percent cover retirees, and 46 million Americans are uninsured.
The problem is structural. Major decisions about health care in the U.S. have traditionally been made by employers, who determine for their employees which benefits and forms of coverage are needed, what types of providers are included in the network, and which organizations administer the benefits. But this paternalistic approach effectively allowed the consumer to be a passive participant in his or her own health care. The consumer has had no economic incentive to seek the best care at the fairest price, or to give up unhealthy habits. Limited competition, unclear pricing, inconsistent quality measures, and complex regulations preserve the disconnect among the three major stakeholders in the system — payers, consumers, and suppliers. This last group includes doctors and other care providers, hospitals, and pharmaceutical companies.
Since 2003, however, the situation has come to seem far less intractable than it once did. That year, Congress enacted legislation that could lead to a transformation of the entire U.S. health-care industry from a wholesale to a retail model, in much the same way that retirement plans moved from defined-benefits to defined-contribution schemes. We’re already seeing early signs of a true retail marketplace:
• New health-care formats and competitors are gaining traction, with MinuteClinics and RediClinics — low-cost walk-in health-care centers for common ailments — at one end of the spectrum, and highly personalized “concierge care” at the other.
• Companies that aren’t traditional health-care players are leveraging their capabilities to create entirely new offerings that enable and encourage the move toward health-care consumerism. Fidelity, for example, is developing products and tools that exploit the emerging health–wealth intersection, such as a calculator that helps predict out-of-pocket health-care costs.
• More employers are starting to offer consumer-directed health plans (CDHPs): high-deductible policies that are usually paired with health savings accounts (HSAs) or health reimbursement arrangements (HRAs) designed to help consumers save money that they can use to offset additional health-related expenses whenever they arise.
• In perhaps the single biggest change, the federal government and leading private-sector payers are driving providers to make cost and quality data more transparent so that consumers can make better-informed choices. Standardized data on cost, service, and outcomes has the power to establish a new basis of competition. Payers are also pushing for new payment mechanisms, such as pay-for-performance, that base reimbursement on outcomes or adherence to broadly accepted clinical guidelines, known as “evidence-based medicine.”
These are promising developments, but not all the pieces that make up a true retail market have fallen into place — and those missing pieces represent real opportunity. Drawing on experience and the insights gained from a 2006 Booz Allen Hamilton study of 3,000 consumers and 600 physicians, we are starting to see which factors will enable the system to work well. (See Exhibit 1.) To make competition and innovation among payers and suppliers possible, the system will require the following: consumers who live healthy lives and plan for their future health-care needs; a fundamentally restructured supply side that provides consumers all the information they need to make wise choices and is quick to respond to changing consumer demands; and new kinds of intermediaries (perhaps the payers of today, perhaps not) to help align the supply and demand sides and help consumers navigate the complex system. All this requires an environment, both regulatory and technological, that encourages innovation and competition. There is tremendous potential for those players who empower consumers in this arrangement, with information, tools, and services that help them take control of their health care immediately and in the future. None of the three — consumers, payers, or suppliers — can drive the changes alone. As with any other market, the system won’t function unless all the elements are moving in harmony.
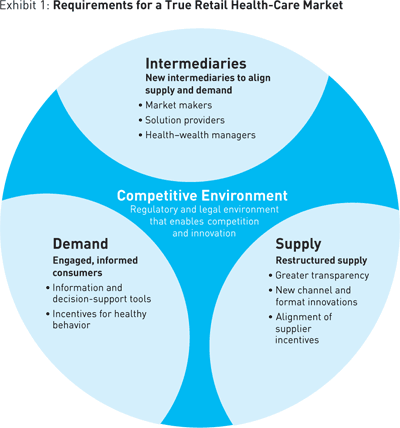
The goals of this retail revolution are to improve health and health care and to transform an annually evaporating asset — traditional health insurance — into a lifelong benefit with real wealth-building potential for consumers over and above any near-term risk management features. New approaches and mechanisms for payment have already emerged, but enormous gaps still exist between the supply and demand sides. Those gaps are where the opportunity lies for players who can bring to market new products and services that align the two sides. The consumer-centric offerings already appearing and those that have yet to emerge are more than cost-cutting tools or cynical antidotes to forced-choice HMOs. They’re probably the last chance for a largely private health-care system in the country.
Consumer-Centrism
Consumerism is not a new phenomenon in the $2 trillion U.S. health-care sector. We’ve seen elements of it, such as direct-to-consumer drug advertising and independent health information sources like WebMD, emerging for more than 20 years. In the last couple of years, however, innovations like CDHPs, tiered drug benefits, and restricted insurance coverage have begun to take hold and are accelerating the retail shift. More than 13 million people, or 7 percent of the population covered by private insurance, are now insured by CDHPs, and the number has been doubling annually since 2004. At that rate, CDHPs in the U.S. will reach the tipping point — generally defined as 15 percent penetration — within the next year or two; once that happens, we’ll see the entire market, including doctors, hospitals, drug companies, or device makers, respond with a more consumer-centric approach, or be left behind.
Informed Decision Making. Much of what is needed on the demand side is in place today or likely to emerge in the near term. CDHP enrollees offer an early glimpse of subtle changes in consumer attitudes in a retail market. Our study shows that CDHP enrollees are more likely to be aware of price and quality differences in products and services and more likely to have seen information and shop around; they’re more likely to ask for prices up front, more likely to negotiate prices, and more willing to trade convenience for lower prices. They’re also more likely to segment health offerings: For those products or services viewed as commodities, they will pick lower-cost alternatives, choosing, for example, generics over branded prescription drugs. They are more likely to plan ahead when making health-care decisions and to invest dollars now to prevent problems later.
But there’s much more to be done to get to a true retail marketplace. Payers and suppliers need a more finely tuned segmentation of customers to reflect their varying degrees of sophistication, needs, values, and financial wherewithal. A retail market requires more comprehensive, trustworthy information and education for consumers. And it needs new kinds of products and services that align with consumer needs to help them become sophisticated and engaged shoppers.
Consumer segmentation in the health-care industry is rudimentary at best. For the most part, payers and suppliers treat consumers as a monolith, with basically the same needs, values, and levels of sophistication. But consumers in any retail market are not homogeneous, and in health care, distinct segments are emerging with different value drivers and varying comfort levels in navigating an increasingly complex health-care market. The industry’s current one-size-fits-all approach to product design, consumer education, and service simply does not work. Clearly, structural change is in order.
Here we can look to innovations in other retail markets for inspiration. (See Exhibit 2.) Leaders in a number of industries leverage sophisticated segmentation capabilities to understand unmet needs across a customer’s life cycle, and then use a strong brand, along with product and service innovations, to drive new demand. Marriott has 10 hotel brands, each with its own business model that appeals to a different segment of the market. Perhaps the most sophisticated consumer segmentation can be found in the financial-services industry, especially in retirement programs. One lesson from the transition to defined-contribution retirement plans is that different customers want help to do different things. Some place greater value on their time than on lowest cost, and therefore hire financial planners to help them prepare for retirement. A self-service segment of the market wants to manage things themselves. And some consumers can’t or won’t manage a lot of complexity, so they are best served by automatic enrollment in 401(k) programs, annuities, and life-cycle funds.
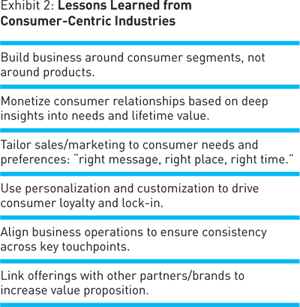
Another insight from retail segmentation is that different consumers need different types of information and education. There are plenty of decision-support resources available and emerging, but they’re not necessarily in formats consumers can easily use, in a language they understand, or from sources they trust. Our study and our experience suggest that consumers have the least confidence in many traditional sources of information, namely health plans, employers, pharmaceutical companies, and the government. They want better communication with their physicians and more user-friendly independent sources, such as Consumer Reports. Those are a start, but the most important step will be standardized metrics and the transparency they offer on cost, quality, and service. The U.S. government is trying to drive this kind of transparency, and has made some progress, particularly with quality measures, but efforts are nascent. We’ll see real progress when consumers and employers join the government and leading private-sector payers in demanding this information.
Some interesting pilots show the direction in which the market for information is headed. Health plans are beginning to offer provider cost and quality data along with decision-support tools. In 2005, Aetna began testing tools that allow consumers to compare physicians on actual cost, so that they can gauge their out-of-pocket expenses. WellPoint has embarked on a pilot program at the suggestion of General Motors to provide complete comparative cost data for hospitals on “episodes of care.” Patients on the GM health plan who are having their gallbladder removed, for instance, can get a cost estimate for every hospital-controlled element of that treatment, including tests, room and board, drugs, and other ancillary services. A growing class of niche players such as WebMD (with its recent purchase of Subimo) are evaluating hospitals and physicians using emerging quality measures, such as error rates and adherence to evidence-based medicine.
Long-Term Incentives for Healthy Living. Along with better information, consumers need stronger incentives to make smart long-term choices about their health. These incentives will come from product innovation — in particular, stronger linkages between employer-sponsored plans and Medicare. We still don’t know whether CDHPs, for example, will encourage long-term behavior change as consumers become eligible for Medicare. The retail market requires incentives that lead consumers toward healthier behavior and toward better management of chronic diseases such as diabetes over both the short and long terms. That will mean aligning employer-sponsored incentives with those in the Medicare program; for example, reducing Medicare contributions in exchange for demonstrated healthy behavior in the working years.
Behavioral incentives have already started to appear. In the U.S., Pitney Bowes has reduced co-payments for diabetes and asthma medications to encourage employees to follow their treatment regimens closely. Taking a page from successful innovations in South Africa, Definity Health has pioneered a “Rewards for Action” program that combines personalized health education with financial incentives tied to getting screenings, treatment, and other recommended care for chronic conditions. Wells Fargo is piloting this program and has already achieved promising early results.
A number of employers, including Safeway and Freddie Mac, are also finding success with wellness programs. Typical wellness programs feature free or low-cost health screenings and other sorts of preventive care, including flu shots. Some of these plans mandate that employees undergo health-risk assessments in order to get medical coverage. These programs pay off in better employee health and reduced costs for both employee and employer.
These pilots are a start, but the industry will need to experiment to find the right approach to providing tailored information and long-term incentives. The private sector can’t do it alone; behavior changes must extend past the consumer’s working life as he or she ages and moves onto the Medicare rolls. It’s already apparent, however, that greater consumer engagement is in turn creating pressures for a different market structure from what we have today.
Reshaping the Supply Side
The supply side of health care significantly lags the demand side in the shift to a retail market. But health-care providers have yet to put significant effort into establishing the enabling conditions that will accelerate that shift: transparency on quality, service, and price; new channels and format innovations; and alignment of provider and consumer incentives.
Transparency and Innovation. Consumers are still looking to physicians to provide the cost, quality, and service information they want, but physicians are not prepared to answer those needs. Our study shows that although most doctors believe that consumerism will have the greatest impact on their practices in the future, relatively few plan to alter the way they serve their patients or to share comprehensive cost and quality data. In a true retail market, suppliers who do not embrace the concept of standardized information on cost, quality, and service will be at a disadvantage. Not only do health-care providers need to make the data available, but they need to use it when they refer their patients to hospitals or other physicians and when they evaluate treatment alternatives.
Standardized measures will enable consumers to pick and choose medical services and products based on the dimensions that matter most to them. We already see competition at the margin in the form of different value propositions. Among the new formats are MinuteClinics and RediClinics, which compete on price and convenience. They’re spreading quickly across the country in high-traffic locations, such as workplaces and stores like CVS, Target, and Wal-Mart. Today these clinics deal with routine needs, like school physicals and sore throat treatment. In the future, they’ll help manage the ongoing needs of patients with chronic conditions.
On a more personalized level, concierge care features doctors who oversee all aspects of a patient’s health care, including advice and treatment, for a flat fee. Today, concierge care is a service mostly for the wealthy. In the future, it may address a broader range of patients; we’ll probably see concierge offerings tailored to children, chronic-disease sufferers, the aged, and other populations for whom the service represents a reasonable value.
Hospitals, too, are devising new formats and products. Some have developed specialties in complex diseases such as heart disease and cancer; greater volume in treating a specific disease often translates into enhanced efficiency and quality of care. Increasingly, the retail marketplace requires that hospitals rethink everything they do to focus tightly on the patient–customer. Hospitals must consider which services really need to be provided within their own walls; whether to relocate certain services, like diagnostic testing, to convenient settings in shopping malls or physicians’ offices; whether to outsource their back-office and other functions, including aspects of radiology; and whether services should be bundled to provide soup-to-nuts care in such areas as obstetrics and orthopedics.
Michael E. Porter and Elizabeth Olmsted Teisberg promote that last scenario in their recent book, Redefining Health Care: Creating Value-Based Competition on Results (Harvard Business School Press, 2006; see “Does Health Care Have a Future?” by Joe Flower and David Knott, s+b, Spring 2007), and we agree it is the best path forward. Porter and Teisberg are correct to note that what little competition there is today on the supply side is at the wrong level: It’s health plan competing against health plan, or hospital against hospital. Competition will work best for all when it takes place on the level of solutions to medical conditions, as in one knee-repair team or one diabetes-care team versus another. If and when that happens, we’ll finally have true competition that gives consumers quality and value.
Advances in Technology and Connectivity. Enabling these changes will be advances in medical technology and health information technology (IT). Connectivity among providers is crucial, as is the ability to monitor and consult with patients from afar. The technology already exists to help monitor chronic conditions from home: Diabetics can test their blood sugar levels using a device that automatically sends the data to their physicians or a third-party monitoring service. Similar technology is being developed for distance monitoring of asthma and cystic fibrosis. Cleveland Clinic now has an electronic second-opinion service on the Internet, as well as a comprehensive e-services product line that provides patients and non–Cleveland Clinic doctors access to an individual’s electronic medical record and test results.
But additional investments in health IT and greater connectivity among providers will be needed to ease sharing of patient health information and enable consumers to better manage their own health. Leading providers have implemented electronic prescribing, electronic medical records, and clinical decision-support systems, but the market is still relatively unconnected — “islands of automation” exist. Connectivity among systems and between providers and patients is limited. Comprehensive interoperability among systems and players is a must for the retail market.
There has been progress on this front. Intel, Wal-Mart, and BP, among others, recently announced a pathbreaking initiative to store digital health records for their employees in a data warehouse linking hospitals, doctors, and pharmacies. This program could be the first step on the path toward giving patients access to their own health records in order to coordinate their own care. The big question here is whether consumers will actually trust employers to have access to their medical records.
Aligning Supply-Side Incentives. In order for the supply side to better align with consumer needs, the right incentives must be in place. The incentives today for health-care providers and other suppliers are simple: Get, keep, and grow your business. Health plans from the private and public sector alike squeeze doctors on reimbursement rates, driving some doctors to bump up the number of patients they see and the number of services they recommend. Furthermore, suppliers have no financial reason to provide patients with the advice and information they need.
Employers and health plans are exploring new payment schemes with strong incentives geared toward providers. Some are experimenting with pay-for-performance programs. At least 100 such programs are in operation today in the U.S., and some have shown promising results. These programs, however, are in their infancy and lack the standardized performance measures, electronic medical records, and connectivity they need to be truly effective.
Strengthening the system’s transparency, innovation, and incentives will reshape the health-care value chain. Existing players will battle new entrants for market leadership roles and will have to reconsider the roles they do play. They’ll need new capabilities and new ways of doing business. Players may need to move beyond care provision or drug manufacturing, for example, to assume a more advisory role, to help consumers align individual demand with supply-side options. Our survey indicates that consumers may be open to new offerings — for example, individualized care management programs and performance guarantees for prescription drugs.
New Intermediaries
The least-understood aspect of the retail health-care market is the fledgling hybrid role that will exist between supply and demand to help consumers navigate the complexities of health care. The players that have traditionally held intermediary roles — employers, government, and health plans — do not inspire trust in consumers, nor do they answer all the consumers’ needs. The new intermediaries will identify consumer needs and steer the supply side to answer them. Further, they will catalyze change as suppliers’ inadequacies become more obvious. Though they have barely started to take shape, these new intermediaries will be a potent force in determining which players succeed and which fail in a consumer-centric retail health-care market.
We’re already seeing entrants in this burgeoning space. AOL founder Steve Case is bringing Revolution Health to market in 2007, after spending hundreds of millions on acquisitions, with an information/community portal, a network of RediClinics, a health concierge service, and a consumer-driven health insurance marketplace. Financial-services companies like Fidelity are also, as mentioned above, moving into this business. They will not be alone.
We see three important intermediary roles in the near future: market makers, solution providers, and health–wealth managers:
• Market Makers. Every large market in the nation will need transparent, objective, and reliable information on pricing, quality, and service. Over the longer term, this arena may evolve to include such features as spot pricing, offering discounts for care at less busy times. Insurers already have skills and databases that they could leverage for such a play, but they will most likely need to partner with third parties that are viewed as more objective and trusted. Groups like the American Heart Association or the American Cancer Society could become market makers for disease information or a seal of approval.
• Solution Providers. Solution providers are emerging to bring evidence-based treatments to consumers, especially to those with difficult, chronic, or expensive conditions. We can see the outlines of a “bundler” role: Instead of offering services à la carte for diseases like diabetes, providers could handle the entire treatment of a disease over a person’s life. In Redefining Health Care, Porter and Teisberg recommend packaging best-of-breed treatments into an easily purchased bundle and then taking responsibility for the result, such as lower blood sugar levels or fewer ER visits. These players will be the masters of disease management, and it is possible to imagine some CDHPs requiring participation in such programs as a condition of continued enrollment. The space will offer some of the most interesting opportunities in the long term, especially for market-leading providers with exceptional skills and experience. Eventually, we can see this role combine with that of the market maker.
• Health–Wealth Managers. Consumer-directed health-care players have focused so far on simply managing health-asset transactions. But as CDHPs gain more traction, health savings accounts will combine with the larger world of wealth management to form an entirely new industry. Financial-services players are likely to dominate, but cobranded alliances with health plans could be powerful. Within this arena, customer service and product innovation — such as offerings that tie in disability and long-term-care insurance — will be critical for success. This convergence of health-care benefits and broader financial services will potentially involve hundreds of billions of dollars and will spark new thinking about the nation’s savings behavior and lifelong wealth creation and management.
At this early stage, it may be tempting to think that there will be one answer in each of these three arenas and that fast followers will be disadvantaged. A more likely scenario is that segmented plays will thrive, each catering to different demographics, diseases, life stages, and wealth levels. Still, the battle for critical intermediary positions will be intense — in part owing to the large financial opportunities, but also because the intermediary role gives suppliers critical access to target customers. How that pie will be divided is still up in the air, but it’s clear it will be shared differently than it is today.
The Competitive Environment
As a market maker and an enabler of change, government plays a vital role in creating the right environment for a more transparent and competitive retail marketplace. But for that environment to function well, federal and state regulations and laws need to enable, not hinder, competition and innovation.
Many of the conditions that helped spark the latest health-care industry product innovations were put in place after the passage of the Medicare Prescription Drug, Improvement, and Modernization Act of 2003. This bill and subsequent policy clarifications by the Internal Revenue Service allowed for the creation of portable and tax-advantaged CDHPs and HSAs. The legislation resembles the 1978 law that enabled the creation of 401(k) accounts.
The federal government, however, cannot reshape the marketplace on its own. Many of the current barriers to competition and product innovation exist at the state level. For the most part, unless employers are self-insured and therefore regulated under federal Employee Retirement Income Security Act (ERISA) employment laws, the states regulate health insurance. Most states mandate which benefits must be included in employer-sponsored insurance plans. These benefit mandates limit product innovation and make the cost of health insurance higher for those companies that are too small or that lack the know-how to self-insure. Employers cannot obtain a no-frills, high-deductible package.
Some states also oversee the construction or renovation of health-care facilities, and even regulate the purchase of high-end medical technology, such as MRI scanners. Although the original intent was to ensure that any region’s health needs were met and to prevent excess supply, the oversight process has become politicized. It tends to protect existing players’ interests, discourage new entrants and innovations, and limit options for consumers, thus reducing competition.
Finally, state laws governing the licensing of clinical professionals also retard the development of new care-delivery models. Although some regulation is necessary to ensure safety, regulations often restrict tasks that other licensed clinicians can perform. For example, in some states, only licensed radiology technicians can perform certain diagnostic tests, even if nurses or others with related skills could be adequately trained to perform these activities as part of a team-based approach. Other state mandates governing staffing ratios and minimum lengths of stay for certain procedures attempt to improve patient safety but also inhibit providers from improving the delivery of care while protecting the jobs of those who helped craft the regulations. For the health-care market to more efficiently and more creatively meet the needs of consumers, these kinds of obstacles need to be lifted.
The Road Ahead
It’s clear that the future of health care in the U.S. will be consumer-centric, but exactly how this will play out is still coming into focus. The evolving model will be influenced by a number of factors, including retail health experiments now unfolding in other countries, as well as by the experiences of other consumer-driven industries such as retailing and banking. What is certain is that the health-care landscape is undergoing a profound alteration that will change the dynamics of all the industries connected to it.
The shifts will create enormous opportunities that will challenge and reward insurers, providers, product makers, intermediaries, and even new entrants. Virtually all of these opportunities are in new or significantly altered competitive spaces. And in each of these spaces are gaps that need to be filled in order to connect increasingly involved consumers with the right providers, in the right setting, at the right time, with the right services, at the right price. When that does happen, we’ll see genuine competition that addresses the affordability crisis, increases coverage for the uninsured, and provides a sustainable private-sector solution for healthcare in the United States. ![]()
Reprint No. 07107
David G. Knott (knott_david@bah.com) is a senior vice president with Booz Allen Hamilton based in New York City. He works with health services clients on corporate and business unit strategies and transformation programs.
Gary Ahlquist (ahlquist_gary@bah.com) is a senior vice president with Booz Allen Hamilton based in Chicago. He specializes in the strategy-driven transformation of insurance companies, health plans, and health providers.
Rick Edmunds (edmunds_rick@bah.com) is a vice president with Booz Allen Hamilton based in Washington, D.C. He specializes in the life sciences sector.
Also contributing to this article were former Booz Allen Hamilton Vice President Phil Lathrop, former Booz Allen Associate Bela Prasad, and Booz Allen Principals Danielle Rollmann and Cindy Vanderlinde-Kopper, and Consultant Jeffrey L. Hung.


