How Engineering Principles Can Improve Healthcare
This four-part approach can help outpatient clinics treat more patients with the same facility and staff.
Here’s a typical day at many hospitals: In the boardroom, the executive team considers how to bring in more patients because the insurers are squeezing prices and competitors are ramping up advertising. On the hospital floor, physicians and nurses rush from procedure to procedure, seemingly without enough hours in their day. Meanwhile, patients sit in the waiting room, growing frustrated (and those calling the hospital sit on hold), even as exam rooms are empty and multimillion-dollar equipment sits idle. What’s going on here?
The issue has to do with the utilization of clinicians, staff, and assets—a problem that’s only going to get worse. Aging populations, the rising incidence of chronic disease, and healthcare reform are leading to a growing demand for care, particularly specialty healthcare such as obstetrics and gynecology, pediatrics, neurology, cardiology, and oncology. Although many of those treatments require inpatient stays, there is a real opportunity to deliver some aspects of specialty care via outpatient clinics and departments within hospitals. Yet in our experience, many such clinics are extremely inefficient in the way they deploy their staff and use their facilities to meet the demand for care. The influx of newly insured patients, combined with the projected shortage of newly qualified clinicians, will only compound this problem.
The solution, we believe, is for specialty outpatient care clinics and departments to better use their current facilities in order to improve access to care. More specifically, hospitals and health systems should apply the proven principles of industrial engineering, through four specific levers.
1. Demand and operations planning. Many specialty outpatient clinics use some kind of demand planning, yet it is often ad hoc and infrequent (typically once or twice a year), and based on benchmark staffing ratios. This is a reactive approach, and akin to driving by looking only in the rearview mirror. Instead, clinics could implement more real-time tracking tools to continuously assess demand levels and better predict surges. Many administrators think they need to buy complex and expensive workforce management systems, but a basic spreadsheet program such as Excel is often good enough to realize the first set of improvements. In addition, clinics shouldn’t rely on external benchmarks or generic staffing ratios but instead develop these parameters based on clinic- or department-specific demand. The goal in this first step is to get a more accurate and up-to-date assessment of demand, on a daily or even hourly basis.
A metric that clinics can use to gauge their performance in demand and operations planning is the percentage of total payroll that is allocated to overtime, or to third-party agencies that provide short-term staff to fill in gaps. High levels in both—combined with periods of low staff utilization—may indicate that the facility is not matching supply to demand dynamically.
2. Talent management. Whereas the first lever looks at the volumes, the second looks at the nature of the services—namely, the current qualifications and training levels of clinic staff. Again, many facilities have some kind of talent management program in place, but it’s administered infrequently, and the responsibilities of team members at different levels tend to blur.
Using a more systematic approach will ensure that the clinic has the right people in the right roles, and that they’re performing at the top of their current qualification level and job description. A key component of managing talent is ongoing training and testing, including clinical refreshers, for staff at all levels. The goal should be to assign tasks according to the education level, expense, and revenue-generation potential of each team member. The result is not only a more efficient operation but a better experience for patients and staff.
Two metrics to measure performance in talent management are the percentage of staff operating at the top of their skill set, and the length of time since the last refresher training session.
3. Patient flow. Typically, the flow of patients through the clinic—from entry to departure—moves in fits and starts, driven by bottlenecks in staffing, rooms, and equipment. To address flow, administrators must redesign the process of care, standardize procedures, automate basic decisions, and make sure that all tasks get assigned to team members with the right skill sets. In our experience, a more standard flow shortens wait times for patients while increasing their face time with the physician, reduces task time and inefficiencies for clinicians, improves the productivity of staff and facilities, and boosts the quality of care.
Two metrics to assess patient flow are the average wait time, and the percentage of clinic time overruns (indicating the degree of overbooking).
4. Scheduling. Once demand, supply, and flow have been addressed, the final component is scheduling, where we often observe two extremes: Scheduling can be mechanistic (aimed at maximizing volume) or highly customized (driven by the preferences of individual physicians). Physicians often insist on the custom approach to avoid the former and preserve continuity of care.
We believe that the best scheduling style does not consist of cramming ever more appointments into a doctor’s day. Rather, it’s intended to ensure that patients get the right appointment type with the right physician, at the right time, and for the right amount of time. Clinics can achieve this by establishing simple decision trees to identify the correct appointment duration, along with implementing standard physician clinic times and clear policies about preregistration. For example, require patients to submit all new-patient data in advance, via email or over the phone.
Additionally, a high-performing call center can take on some of the administrative functions that are now typically handled in the clinic, such as performing basic triage to schedule appointments, resolving billing disputes, handling reminders, and helping patients manage chronic conditions through the use of online monitoring tools.
Three metrics to assess scheduling performance are the average number of days before a patient can get an appointment, the percentage of time the patient gets to see his or her preferred physician, and the no-show rate.
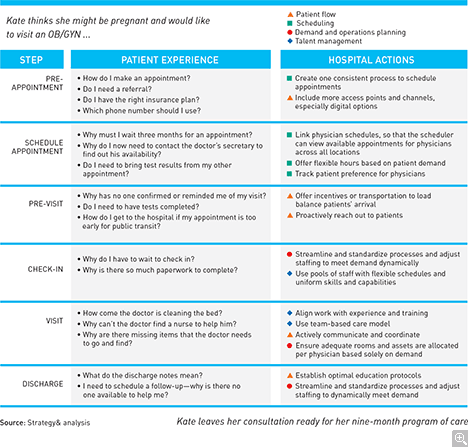
Although each clinic or outpatient department will likely focus on one or two levers, success will come only from addressing all four simultaneously (see Exhibit). Moreover, it’s critical to get doctors engaged in the process as early as possible. If the initiative is structured around the patient’s experience and continuity of care (rather than just productivity), physicians will become champions. And at that point, physicians can begin working with administrators, and also the rest of the staff, to design and implement the right solution. (Fixes imposed from above in settings as complex as specialty outpatient care usually lead to failure.)
Already, a number of clinics have used this approach and generated solid results. For example, a health system recently improved its patient volumes by 20 percent in a financially sustainable way, including better access for the uninsured, with no changes to the facility or staff levels. The health system also improved its quality of care, patient experience, and staff engagement—getting the right results in the right way.
Through this method, a health system recently improved its patient volumes by 20 percent.
Similarly, a clinic with five specialties synchronized the weekly schedules of 20-plus clinicians and matched room assignments with patient demand. The result was a 50 percent improvement in access. And a large academic medical center identified a laundry list of opportunities across 14 ambulatory specialty care clinics and departments. It is now in the process of implementing the four levers to expand access by up to 40 percent while reducing the labor cost per visit by 20 percent.
Although some may debate the reforms currently under way, improving access to outpatient specialty care is something virtually everyone can agree on. By adopting this approach, which has already proven its merit, clinics can better connect patients with physicians, improve the quality of care, empower nurses and other staff members, and help the hospital reduce costs. ![]()
Author profiles:
- K. R. Prabha is a Strategy& senior associate based in San Francisco.
- Igor Belokrinitsky is a Strategy& partner based in San Francisco.
- Strategy& associate Jo Lim also contributed to this article.