The Innovation Sandbox
To create an impossibly low-cost, high-quality new business model, start by cultivating constraints.
(originally published by Booz & Company)
 |
|
Illustration by Dan Page |
Not far away, prototypes of a multiple-fuel stove for the rural poor are being tested by a large multinational corporation. The potential consumers of this stove typically use cow dung and biomass (sticks and grass) for cooking fuels. These fuels are inefficient, and the smoke from indoor fires can be harmful. With the “combination chula” (chula is the Hindi word for stove), a housewife can switch from biomass to natural gas instantly, depending on her budget and priorities (for example, whether she is cooking dinner for family or making tea for an unexpected guest). The cost of the combination chula is less than 1,000 rupees (about US$20). If it succeeds in India, it will be rolled out across multiple geographies, with potentially immense impact on the quality of life of people throughout the developing world.
Innovations like these are not just technological or market breakthroughs. They change people’s lives. The hotel, by facilitating travel for many more businesspeople, could greatly expand commerce in India. The stove could improve the lives of millions of people. The process for designing both of these breakthrough innovations started with the identification of the following four conditions — all of which are difficult to realize, even when taken one at a time:
-
The innovation must result in a product or service of world-class quality.
-
The innovation must achieve a significant price reduction — at least 90 percent off the cost of a comparable product or service in the West.
-
The innovation must be scalable: It must be able to be produced, marketed, and used in many locales and circumstances.
-
The innovation must be affordable at the bottom of the economic pyramid, reaching people with the lowest levels of income in any given society.
In countries like India, with 700 million bottom-of-the-pyramid consumers at varying levels of income, the need for innovations that meet these criteria is now becoming obvious. The seemingly impossible demand of a hitherto unserved customer base — a $20 hotel room in an environment of $250 to $300 hotels, or a cookstove for use by an impoverished villager — became, in this case, a specification for starting the innovation process.
This approach could be called an innovation “sandbox” because it involves fairly complex, free-form exploration and even playful experimentation (the sand, with its flowing, shifting boundaries) within extremely fixed specified constraints (the walls, straight and rigid, that box in the sand). The value of this approach is keenly felt at the bottom-of-the-pyramid market, but any industry, in any locale, can generate similar breakthroughs by creating a similar context for itself. In India, several such breakthroughs are taking place now, in a global industry that is otherwise plagued by high costs, stultified traditions, a variety of regulators, a perennially dissatisfied customer base, and a reputation as an exceptionally difficult venue for business innovation. That industry is health care.
Bypassing Conventional Approaches
As a demonstration of the opportunities for breakthrough innovation, the health-care industry in India is ideal. India is known for its dismal state of public health, the spread of HIV/AIDS, and high rates of infant mortality. The country has more than 6 million blind people and more than 50 million malnourished children. Type 2 diabetes (with related illnesses such as ischemic heart disease) has reached epidemic proportions, with an estimated 100 million patients expected by 2015. Meanwhile, more than 80 percent of the population cannot afford the costs of health care; insurance is unavailable to most of them.
Finally, more than 490 million people (about 70 percent of the Indian population) live in rural and semi-urban areas. They are difficult to reach, especially in a country where doctors are scarce (the ratio of physicians to total population is less than one per 100,000 people, compared with about one per 160 in the United States). World-class facilities are even scarcer. Rural patients must often travel to cities for treatment, a journey of excessive cost since their family members travel with them. These constraints affect the nature of health care in unexpected ways. For example, in the United States, a customized lower-limb prosthetic may require several fittings spread over weeks. In India, it must be finished in one eight-hour sitting, so the patient and his or her family can return home before their money runs out.
And yet amid all these constraints, a few health-care providers in India are establishing new global standards for cost, quality, and delivery. They do it by bypassing the conventional approaches to medical practice. For example, the Narayana Hrudayalaya cardiac care center, located in Bangalore, is one of the world’s largest providers of heart surgery and other forms of cardiac care, including care for children. A private corporation, it was founded in 2001. Only three years later, in 2004, the company performed 7,500 cardiac surgeries and treated 60,000 outpatients, including almost 2,000 telemedicine patients who received consultation and treatment at remote sites, accessing specialists through satellite- and Internet-based telecommunications links.
It’s important to note that the facility and its parent company, Narayana Hrudayalaya (NH), are profitable. And NH’s cardiac care is far from the only profitable health-care innovation emerging from India. The most famous example (documented at length in my book The Fortune at the Bottom of the Pyramid) is the “Jaipur Foot,” a prosthetic foot made from rubber, intended for below-the-knee amputees, such as people injured by accidents and land mines. The JF (as it is universally called) costs about $30, a fraction of the $8,000 to $10,000 cost of a similar Western prosthesis; if a patient damages, loses, or outgrows it, he or she can simply get a new one. Since 1975, the JF has been distributed by a nonprofit, nondenominational organization called the Bhagwan Mahaveer Viklang Sahayata Samiti (BMVSS), which fits about 16,000 patients per year, with trained paramedics as the primary patient contact. BMVSS also ships artificial feet, calipers, and other aids to thousands of patients worldwide — more than 50,000 in 2004. BMVSS does not charge for its prosthetics and service; it survives on donations from satisfied patients and from philanthropists.
Another example is the Aravind Eye Care system, the world’s largest provider of cataract surgery. This company, founded in 1976, performed 240,000 surgeries in 2004 and treated 1.6 million outpatients. The founder, Dr. G. Venkataswamy, has said that his goal is to “wipe out needless blindness.” Thus, Aravind treats more than 60 percent of its patients free — and continues to operate profitably.
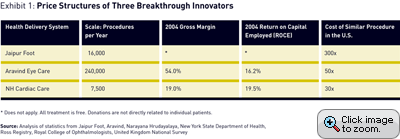
All three health-care innovators, NH, BMVSS, and Aravind, have been around long enough to give us confidence that these innovative health-care efforts represent sustainable businesses. The basic performance of these three systems is captured in Exhibit 1.
Faced with the difficulties of an emerging market like India, health-care managers can easily give up. They can conclude, as many development experts have, that the only way to provide good-quality care at the bottom of the pyramid is through public-sector subsidies and through philanthropy. Often, this leads to few variations on existing products or services.
But suppose we started instead with a simple premise: The poor deserve the same quality of care the rich get. Keeping world-class quality as a nonnegotiable standard allows us to challenge many assumptions regarding cost, quality, and delivery. That, in fact, is what JF, Aravind, NH, the indiOne hotel chain, and the producer of the combination chula have in common: They are innovating within a set of self-imposed constraints, derived from consumer insights that other innovators have ignored.
The Sandbox in Action
Exhibit 2 represents one sandbox: the constraints and innovative activity for the health-care industry in India. There is no generic sandbox design, any more than there could be a generic checklist of strategies that would apply to every business. For each combination of region and sector — such as hotels, stoves, or health care in India — leaders start by identifying the core constraints that they must overcome to achieve a breakthrough innovation. The constraints are like the limits on an ecological niche, prodding the evolution of new products and services. For the health-care industry in India, the constraints were world-class quality, new price performance levels, scalability, and universal access (availability for people in rural areas in particular). If the sandbox diagram showed the hotel industry, some constraints would change: Price performance (value) would probably remain, but universal access might be replaced by modernity and aesthetics. A concerted effort is needed to identify these core constraints; there may be more or less than four in some cases, but there should not be many more (or less). Then, once the sandbox is defined, it can force unconventional thinking in several directions at once.

1. Specialization. Although the basic unit of health-care delivery around the world is a general hospital, the successful innovators in India have all specialized: JF in prosthetics, Aravind in eye care, and NH in cardiac care. Specialization allows these organizations to make the most of their resources: people, training, work process designs, capital equipment, and the requisite investment of time and skill for patient acquisition. Specialization also allows each organization to build a unique brand identity that attracts patients, motivated health-care professionals, and donors. Most importantly, the focus on one particular category of service builds expertise that a more general organization could not match. NH performs 23 cardiac surgeries per day; a large urban hospital elsewhere could perform a maximum of four or five. The combination of specialization and volume allows NH to train its doctors and nurses to become experts in a very short time.
2. Pricing. Affordability is critical for both the business model and the underlying vision of service. NH makes no distinction among the quality of service delivered to different patients. Everyone is charged a fixed rate per surgery of $1,500 — one-thirtieth the $45,000 that a typical U.S. hospital might charge, and one-third of the $4,500 that a top-line hospital in India would charge. Even so, many patients cannot afford this surgery; thus, with the help of the ICICI Bank Ltd. (India’s second-largest private bank) and the state government of Karnataka, NH designed a health insurance plan for the poor, selling it to entire villages at one time, at a cost of 20 cents per person per month. More than 2 million subscribers belong to the scheme.
The surgeries are designed with whatever elements are necessary to allow NH to meet the price consumers can afford and still make a profit. This “consumer-generated” approach represents a big change for most managers, particularly in health-care institutions. They are more accustomed to basing their price on the industry-established cost, plus profit. But with a ceiling for costs determined by customer needs, breakthrough innovators are driven to play more effectively in the rest of the sandbox, redesigning their processes as needed to meet those cost requirements.
3. Capital Intensity. In health care, innovators seeking breakthrough cost reductions must focus on reducing capital intensity. Specialization allows NH, for example, to purchase only medical equipment related to cardiac care, and to use that equipment around the clock — typically in three shifts. Off-peak use is further encouraged by incentive; the hospital charges patients less if they come in for tests during odd hours.
Medical innovators in India continually search for ways to reduce the fixed and variable cost structure of their products and services. Jaipur Foot is particularly inventive at this. For example, JF uses commercially available, inexpensive ovens for such specialized tasks as shaping plastic pipes. The raw materials for each prosthetic total about $12.50.
Breakthrough innovators are willing to pay more in fixed costs (like those for equipment) if it means lowered variable costs over time. NH buys digital X-ray machines that store images in computer files; the extra cost is justified by the eliminated costs of X-ray film, storage of old images, and transport of images to remote locations. NH also recruited a local manufacturer to produce its own sutures customized for each doctor at $90 each, compared with mass-produced imported sutures at $200. Similarly, Aravind produces its own intraocular lenses (used in cataract surgery) for $3 each, instead of importing them for $60 to $100 each. The quality is so good that Aravind now exports 50 percent of its production to the United States and other countries.
To accomplish this kind of cost reduction, providers must be willing to look outside conventional industry structures. For example, most Indian hospitals pay the same prices as their American or European counterparts for machines and devices like stents, heart valves, and pacemakers. Yet the technology behind much of this equipment is often rudimentary by today’s standards. EKG, X-ray, and CT scan technologies are all more than 40 years old; their cost is kept high because there are only a few suppliers. Using software and manufacturing capabilities available in India today, innovative medical facilities are encouraging entrepreneurs to enter the medical instrumentation and supply business. The early results suggest that Western medical equipment manufacturers will soon face severe competition from Indian “format invaders” — new entrepreneurs using their cost advantages to reframe the value proposition of an established global industry.
4. Talent Leverage. Operating amid a scarcity of trained medical practitioners (India trains only 80 cardiac surgeons per year, whereas the U.S. trains 8,000), breakthrough innovators in Indian health care have had to focus on the skills they need rather than the credentials of their staff. They have stumbled on a critical insight: The more involved they become in building the skills of their people, the more effective they can be at providing world-class service while holding down costs.
Surgical skills, in particular, are improved by frequency of encounters. No surgeon can keep pace with all the subspecialties in the field. Therefore, by disaggregating the medical process, a medical institution can make far better use of its higher-credentialed physicians.
Dr. Devi Prasad Shetty, chairman of NH (and a well-respected surgeon), explains the logic this way: “The task of heart operations has been broken into many tasks. Each is managed by a group of professionals. One of my colleagues conducts most Dor procedures — a complex left ventricular remodeling procedure that is done by only a few experts all over the world. Since he has completed more than 250 of these, we all refer patients for this procedure to him. Similarly, everyone refers patients who need the Ross procedure to me, since I have conducted more than 150 of them with zero mortality. Because we deal so frequently with so-called rare procedures, it is not difficult to standardize them and consistently get good results.”
Meanwhile, NH recruits women with high school educations and trains them as echocardiographers; they produce excellent results because they do nothing but read images, as many as 200 per day. In most facilities, as Dr. Shetty notes, “Echocardiogram tests on children are conducted by senior pediatric cardiologists. However, there are very few pediatric cardiologists in India, and they are required for other tasks: interventions and managing children before and after the surgery. So we created a parallel team of echo-technicians, nongraduates to whom we give extensive training. They work from morning till evening every day, with a lot of passion, because this occupation has given them a new status in society. Of course, senior doctors supervise their work. But because they are so specialized and attentive, it is not uncommon for us to detect an abnormality of the heart during an echocardiogram conducted by a technician, when it was missed in other institutions by cardiologists.”
5. Workflow. In a typical hospital, a cardiac surgeon admits the patient, orders tests, synthesizes the resulting information, plans the surgery, coordinates the team, and monitors postoperative care. The surgeon, in short, is treated like the conductor of a complex orchestra, with responsibility, as an individual, for the overall outcome.
By contrast, at NH and Aravind, surgeons specialize and the team is responsible for outcomes. At Aravind, a surgeon moves from one operating table to another, focusing on just the procedure, while teams of two nurse-practitioners remain at each table and oversee the patient’s care. Process design is critical: The quality of the outcome depends on the sophistication with which the total task has been disaggregated and specific credentials and skills have been applied. Each member of the team knows what needs to be done. Individual participants — anesthesiologists, perfusionists, operating-room nurses, and the surgeons themselves — are constantly learning and using their reservoir of expertise to make the appropriate adjustments to reflect the needs of a particular patient in a specific context. They continually improvise, like players in a jazz band.
6. Customer Acquisition. The success of this business model is based on volume. Aravind, JH, and NH must continually attract patients to travel to them. Thus Aravind organizes about 1,400 one-day “eye camps” per year in villages across south India. Teams of doctors and paramedics trained by Aravind visit these camps and screen the assembled patients to identify those who need surgery or other kinds of hospital-based treatment. These individuals are taken to the hospital, often free of charge, with a relative accompanying them if necessary. They are provided food and lodging near the hospital. Nobody is denied access to care. Through this process, which has been gradually augmented by telemedical examinations, Aravind screens more than 1.6 million people per year. This yields 240,000 surgeries.
NH has an even wider catchment area: the Indian states of Karnataka and West Bengal, covering more than 60,000 square miles. NH is organizing cardiac care units at district medical facilities throughout these states, with young doctors and paramedics who are trained in cardiac diagnosis and care. If the local experts detect any abnormality that they cannot treat, they can connect with NH through a “tele-link” with two video monitors: one for reviewing medical data and the other for discussing the patient’s condition with the patient and his or her family. Even in this early stage of development, NH conducts more than 350 remote consultations per month. If a patient needs surgery, he or she is advised to go to the main hospital in Bangalore.
7. Values and Organization. It is not possible to understand the breakthrough innovations in these cases without explicitly recognizing the importance of deeply held values. Everyone who works at NH, for example, is imbued with the same purpose: to provide all people, rich and poor, with world-class care.
Because they have these mutual aspirations, teams of people with diverse backgrounds and accomplishments can organize themselves to work together, without needing expensive supervision. Young women from villages, trained as nurses, work side by side with Western-educated doctors at Aravind, designing their processes together.
To provide direction in this type of self-organizing system, the goal must be clear, motivating, and easy to share with a wide range of people. But the means of achieving that goal are never fully delineated; people continually discover new ways of improving their service. The overall culture is one of service, humility, kindness, and equality. Or as one doctor at Aravind put it, “All the doctors speak softly to the patients and nurses. No shouting here. If a doctor behaves in an unacceptable manner, word goes around the hospital in no time, and the doctor will be in trouble. We believe in mutual respect as a core value.”
The Innovator’s Ecosystem
It is easy to copy a particular innovation from any of these organizations. For example, another hospital might mandate a three-shift schedule for an expensive piece of equipment. But the savings will not be realized by any such measure alone. NH, Aravind, and JF succeed because they continually innovate with a “sandbox” approach, and continually convert these innovations into disciplines and protocols that spread throughout their entire organizations. Training and skill-building are integral parts of their operations.
Because they meet complex needs with specialized organizations, breakthrough innovators tend to discover that they cannot operate alone. They need to form alliances with a group of interrelated organizations — in effect, creating an ecosystem for breakthrough innovations. For example, the Aravind ecosystem includes five hospitals in the southern state of Tamil Nadu; a medical research foundation; two research institutes; Aurolab (a lens and suture manufacturing company); dozens of community outreach programs; and relationships with universities (including some in the U.S.), governments (at a variety of levels), and technology providers. NH could not operate without its alliances with ICICI bank, with a wide range of low-cost suppliers, with state governments (which allow NH to use government hospital premises to site its cardiac care units), and with the Indian Space Research Organization to get satellite availability for telemedicine. The ability to develop these relationships to deliver high-quality care represents an important competitive advantage.
India is not like Silicon Valley today, where infrastructure and relationships, including those with nearby universities, are already in place, and a new company plugs into them. Here, they must be created from scratch. For example, only after it became clear that patients could not afford the $1,500 price tag for surgery did NH conceive of low-cost insurance; and only then did the company approach the ICICI Bank. By playing the role of a core node in a larger network, NH provided both an intellectual influence and a venue (the “sandbox”) in which others could take part. NH dictates the standards, controls the way people engage with its system, and maintains privileged access for itself. But it does not own or control all the participating organizations, nor does it need to.
Companies in any industry, in any country, can adopt a “sandbox” approach to breakthrough innovation. But it requires accepting a few premises that are counterintuitive to many managers:
• They must radically rethink the entire business model — technology choices, distribution, pricing, scale, workflow, and organization. Fine-tuning the existing business models will not work. That is why the bottom-of-the-pyramid customer base is the best friend that a company focused on breakthrough innovations ever had. This unfamiliar market with very low discretionary income provides sufficient distance from the current top-of-the-pyramid customer base to force institutions to change their practices.
• Rather than researching markets, they must immerse themselves in the lives of their target consumers. At the bottom of the pyramid, there are tough challenges in access, awareness, affordability, and availability, and only those who are grounded in the reality of their consumers’ lives will understand their priorities. The consumers themselves may not articulate their needs.
• They must accept constraints. They cannot do all things; they must do a few things very well. Many people have come to believe that creativity must be unconstrained; in practice, however, breakthrough creativity requires an explicit acknowledgment of limits.
• They must not innovate in isolation. Breakthroughs occur when there are clusters of innovations, taking place continuously over time, in small experiments from which companies learn rapidly, and in an ecosystem involving many collaborators and partners.
• None of these changes will be possible without a clear and unflagging commitment to a strategic intent. In the case of Indian health care, that is the intent of serving all people with world-class quality at prices they can afford. Guided by that value, the process of breakthrough innovation is a market development task; it is very different from the challenge of serving an existing market more efficiently.
Other industries may use other constraints to achieve breakthrough innovation; for example, as companies become more aware of the problems of global climate change, they are increasingly willing to innovate toward formerly “impossible” goals of generating no toxic waste, contributing no potentially damaging effluents to the atmosphere, making efficient use of energy and natural resources, and restoring health to land and water. These external constraints now become resources for internal creativity.
Or consider the clothing chain Zara, which turned the fashion industry’s supply chain model upside down. Traditionally, clothing suppliers have forecast what customers will want, produced large lots, and provided them to retailers with a lead time of several months. Zara accepted the constraint of immediate responsiveness. It makes small quantities of any item, and provides the items only about 10 days after they leave the designer’s desk. The link between customer response and the next wave of design is extremely short, so Zara’s risks are vastly diminished. Its managers need not worry about misperceiving their audience. This frees them to put excess capacity where it is most needed: in trucking, fabrication technology, and other aspects of its ecosystem.
Why do multinational corporations find it hard to embrace these approaches? The answer may lie in the dominant logic of successful companies: the business practices that have been successful in the past, the mind-set tied to those old practices, the internal evaluation systems that reinforce this mind-set, and the daunting problem of lack of experience in the new way of operating. The zone of comfort drives away the zone of opportunity. If managers believe that 80 percent of humanity is “too poor to pay for our products and services and is not part of our target market,” then a new offering at one-fiftieth the price of the current offering, made without sacrificing quality and at the same time ensuring the company’s profitability, looks at first glance like an impossible task. So those managers assume that the idea will be impossible; instead, they make minor changes to existing products and business models, start endeavors that often fail, and conclude from those failures that success was indeed impossible.
Managers who want breakthrough innovation need to build a new capability for it in themselves. The opportunity beckons. The bottom-of-the-pyramid consumers are ready. All that remains is for the companies to mobilize themselves accordingly.![]()
Reprint No. 06306
Author profile:
C.K. Prahalad (ckp@umich.edu) is the Paul and Ruth McCracken Distinguished University Professor of Corporate Strategy at the University of Michigan. He is the author of The Fortune at the Bottom of the Pyramid (Wharton School Publishing, 2005), and coauthor (with Gary Hamel) of Competing for the Future (Harvard Business School Press, 1994).