Health Care's New Electronic Marketplace
First came self-managed 401(k)s. Get ready for self-managed medical plans and the multibillion-dollar Internet marketplace they will spawn.
(originally published by Booz & Company) Over the next 10 years, employer-sponsored health plans will evolve en masse into defined-contribution formats, finally and irrevocably creating a consumer-driven health-care system in the United States. Much as the deined-contribution model has put individuals at center stage in determining how to finance their own retirements, employees will soon be placed in the driver's seat for selecting their own health plans in an open market.
Over the next 10 years, employer-sponsored health plans will evolve en masse into defined-contribution formats, finally and irrevocably creating a consumer-driven health-care system in the United States. Much as the deined-contribution model has put individuals at center stage in determining how to finance their own retirements, employees will soon be placed in the driver's seat for selecting their own health plans in an open market.
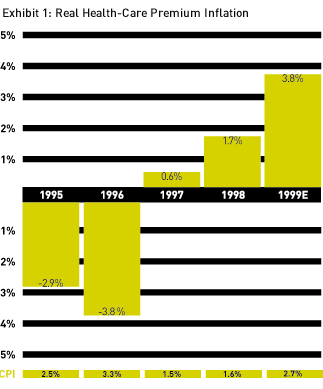
Economic, political, and social forces are starting to converge, and a public dialogue is developing. Health-care premiums, briefly under control in the early- and mid-1990s, are once again outpacing the consumer price index. (See Exhibit 1.) Seeing this, employers who participated in a Booz-Allen & Hamilton survey of leading companies express a nearly universal readiness to embrace new health-care benefits approaches that would limit their exposure to rising costs, and return choice and accountability to employee-consumers. Republicans and Democrats alike have presented election-year proposals addressing issues of access and cost via expanded enrollment in public risk pools (e.g., the Federal Employees Health Benefits Program, or FEHB, and Medicare), continued tax deductibility of benefits, and even tax credits. All of these point to a defined-contribution approach. The recent success of similar changes in retirement benefits also augurs well for a fair hearing from consumers.
Health Care's Power Retailers
The underlying idea is simple, but the implications are profound. The supply side of the health-care industry will see the emergence of new business models, notably power retailers who use the Internet to create vast, Toys "R" Us-style health-care superstores. In this environment, all existing industry participants will need to become more consumer-focused. In addition to battling the newcomers, today's health-plan providers will have the chance to integrate functions that can lower the costs and risks of developing new sales channels and customer-friendly services. Changes in the marketplace will also open opportunities for outsourcers.
Accelerating double-digit growth in health-benefits costs is once again becoming a reality for some employers. Under these circumstances, our survey of leading companies suggests that employers will welcome the opportunity to limit the risk of future health-benefits cost increases, eliminate much of today's embedded infrastructure costs, and move out of the thankless role of de facto intermediary between patients and health-care providers. Employees will not lead the defined-contribution revolution, but will find much to like once the concept takes hold.
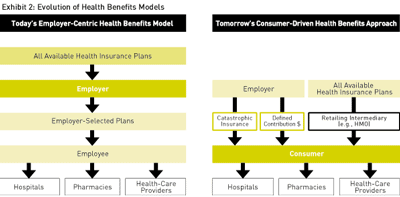
On a practical level, it would work like this: An employee, armed with an annual, defined contribution from his or her employer, would access an online retailer of health benefits — a waiting-to-be-born entity we call "HMOsRUs.com" — and make a plan selection based on the features, risks, and pricing that best meet the employee's needs. (See Exhibit 2, above.) If married, the employee might well combine benefit dollars with those of the spouse and select a single plan for their family. This could free up money for other benefits, such as a contribution to a medical savings account. The online stores would take care of enrollment, card issuance, provider selection, and other front-end services.
Still, the transition to defined-contribution health plans will be more complicated than the conversion of pension programs was over the past decade. The information requirements to provide an open and rational marketplace for health-care benefits (e.g., provider panels, coverage, family structure complexities, high-quality data, etc.) are staggering. In addition, new concepts of risk and non-employment-based group-identity structures will challenge traditional underwriting approaches.
The magnitude of the change brought about by a shift to defined-contribution health benefits will ultimately create new winners and losers in the industry. We estimate that about $18 billion of current spending is up for grabs: the $5 billion health plans spend in sales and marketing; the $3 billion paid to benefits consultants for design, selection, and other services; and the $10 billion employers spend on internal administrative costs — a hidden, often-overlooked burden that adds roughly 10 percent to the $100 billion paid annually in employee premiums and claims.
The economic rewards for rationalizing these distribution, channel, and complexity costs clearly will be enormous for those who own pieces of the answer. Some $200 billion to $400 billion in implied market capitalization may be in play. With so much at stake, senior executives at health plans, health-care providers, and other key players must ask and answer the following questions: When will the shift happen? How? And what can I do — now — to win?
Consumers Rule
For most Americans, health-care coverage and employment are inextricably linked — so much so that the system seems integral to, and eternal within, the workplace. In fact, the connection between health care and employment is a post-World War II phenomenon that has evolved in three stages:
1. The Post-War Supply-Side Surge (1945 to 1967) was based on government initiatives to expand, modernize, and urbanize health care. Massive programs to build hospitals and increase the supply of doctors started in the late 1940s and continued through the 1950s and 1960s. Pre-tax funding of employee health benefits led to widespread insurance coverage.
2. The Great Society Era (1967 to Mid-1980s) worked hard at improving financial access to the system via Medicare (for the elderly) and Medicaid (for the poor). It worked — sparking over a decade and a half of expansion of the supply side as well. However, expensive medical advances combined with Vietnam- and OPEC-driven inflation created a cost crisis.
3. The Transition to Managed Care (1980s to 1990s). Health maintenance organizations (HMOs) arose in response to the cost crisis. The idea was that HMOs would actively manage health-care delivery and associated costs. Although managed care was somewhat successful in slowing the rate of increase in health-care costs, consumers resented having less flexibility in choosing their doctors. Choice became the dominant theme in the national dialogue.
It is this growing demand for choice that is sowing the seeds for the coming health-care revolution, the period we call "Consumers Rule." Frustration with restrictions on choice, continued fragmentation of service providers, and confusion over options, costs, and quality will stimulate consumer demand for all manner of information services. The Internet and e-commerce capabilities will provide that information, and then the sales and fulfillment mechanisms will create a more open market in health-care benefits and services.
Campaign Issue
This year's presidential election has refocused the public's attention on health-care reform. Although the candidates' proposals differ, all seem motivated by three related concerns: rising costs; coverage for the uninsured; and consumer frustration with complexity and perceived limits on choice. No one expects government to mandate a defined-contribution approach as a solution, but candidates are clearly intent on raising the stakes of a nascent public dialogue, and the features, structure, and incentives under discussion are consistent with, and friendly to, defined-contribution mechanisms.
One of President Clinton's recent proposals would retain and enhance the tax deductibility of health benefits and encourage the development of benefits purchasing groups for small businesses (even offering tax credits). Other proposals suggest expanded medical savings accounts, and allowing the uninsured (or the unhappily insured) to buy into the FEHB or Medicare. Translated into the new paradigm, these suggestions hold the promise of decoupling health benefits from a specific employer/employee relationship (i.e., allowing the portability of health benefits); creating risk pools that minimize the specter of draconian, individual underwriting; and retaining or extending the tax incentives that enhance affordability for all parties.
Although the right political climate can enable this change, it will be the employers who catalyze the shift to defined contribution. Social and political pressure to curb rising health-care costs notwithstanding, the structural inefficiencies in health-plan design, sales, and administration are themselves enough to fuel a massive change in funding and distribution models. We anticipate the transformation taking place in the following sequence:
- Phase 1: Employers, burdened by excess administrative costs, will logically deem their annual health-benefits budget as essentially a defined contribution. This will become more prevalent as employers realize that funding a benefit need not require them to go into the market, find appropriate products, run through an annual selection process, and operate ongoing expediter and ombudsman functions.
- Phase 2: Today's health-care benefits Web sites can and will evolve into e-tailers of health-care plans. Although a few sites currently offer individual plan sales in select states, most first serve as platforms for employees to select from among a limited set of pre-approved plan options, and then provide enrollment and other front-end services. True e-tailing, however, is likely to resemble the early days of Charles Schwab & Company's online efforts in the investment world, with Web-based retailers offering a wide variety of their own and other companies' products, lots of information, and low-cost transactions.
Employer Equation
Let's look in detail at the employer side of the equation, since the first shots are likely to be fired from that direction.
Employer-sponsored major medical coverage became commonplace in the 1950s and 1960s. By the 1980s, however, crippling health-care cost increases propelled much of the country to look for a new approach to managing health care. The solution was managed care, with its utilization controls, preferred providers, and increased emphasis on prevention. Managed care seemed to be an answer that worked, resulting in several years of significant reductions in the rate of cost increases. However, it came at the price of consumer choice and with overtones of Big Brother interfering in the patient–provider relationship.
Enter the new managed care of the mid-1990s with its opt-outs, point-of-service features, state-mandated minimum stays, and other expensive variants. Suddenly, this new managed care looked an awful lot like the old indemnity system. Costs went up to fund new features, and complexity now threatens to overwhelm us all. Much of this renascent dynamic has been disguised by the United States' unprecedentedly buoyant economy. Yet we are only a bump in the road away from overcoming these vexing issues.
A Booz-Allen & Hamilton survey of one-third of Fortune magazine's "100 best companies to work for" found all anticipating health-care cost increases of 5 to 9 percent during the coming year, well above the rate of inflation. However, most of these companies (which ranged in size from 60 employees to over 200,000, and included not-for-profits, manufacturing firms, service companies, and high-tech players) characterized this growth as "modest."
Where do they stand on defined contributions? All but a few of the very largest, most paternalistic respondents were anticipating a shift to defined-contribution systems. Fully two-thirds were convinced that defined-contribution health plans were in the offing, but were unwilling to be first movers because they feared alienating employees whom they believed had ample alternative employment opportunities. Ten percent, all large employers, could be characterized as champing at the bit to make the transition to defined contribution, but hesitant to move first until something changes.
Such hesitance argues against a scenario of gradual evolution into a new, defined-contribution system. The risk of alienating employees in a high-employment economy is just too high. The status quo is further reinforced by an entrenched employee-benefits bureaucracy, which will fight to maintain its primacy within the current system. However, our survey indicated that any one of several changes could send the clear majority of the companies we polled in search of new approaches to health-care benefits provision.
First and foremost, a general recession in the economy could quickly and decisively change employers' attitudes toward their work forces from "we're lucky to have these folks" to "these folks are lucky to have jobs." In an environment of layoffs and limited re-employment opportunities, companies would be much more willing to entertain changes and even reductions in their benefits plans.
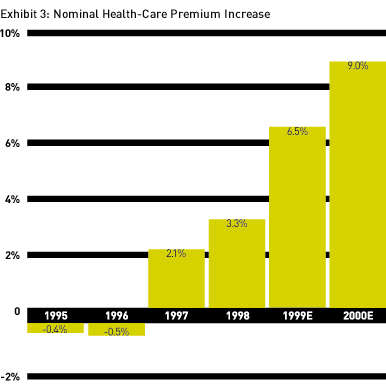
Seemingly intractable benefits cost increases will also push many employers over the edge. Although sanguine about the "moderate" recent annual premium increases (see Exhibit 3, below), companies are unlikely to be comfortable with many more years of medical inflation outpacing the CPI. Finally, onerous additional ERISA mandates or loss of ERISA protections could send many of the nation's largest employers back to the benefits drawing board.
Our conclusion from the survey is that defined-contribution plans will emerge rapidly, but only after a major shock to the economic system, or after cumulative but more moderate changes across the spectrum of employer concerns. That there hasn't been much activity to date is not a sign that the issue is dormant, because we expect the change to occur like a wave that builds and then breaks. Exactly when the defined-contributions wave will break is impossible to project, but it's probably no more than three to five years away.
Complex Solution
Consumers have shown themselves capable of far greater responsibility and independence than many once thought. The rapid acceptance of defined-contribution retirement plans and the increasingly sophisticated use of e-commerce is stunning. The long bull market has certainly helped ease individual investors' downside worries, but even without it, the very concept of defined-contribution retirement plans and the business systems that make them possible must be judged an unqualified success.
Yet it's unlikely that consumers will accept as readily a defined-contribution paradigm in the health-care arena. For one thing, there are few, if any, reliable and accepted performance and quality standards that can guide consumers. Even more significant, retirement planning for most is done with longer-term time horizons in mind. In contrast, the consequences of consumers' health-care decisions are more immediate and potentially more profound, a fact bound to render most more cautious, if not downright conservative.
Perhaps the biggest barrier to overcome is one of conceptualization and expectation. Changes in the health-care system over the past two decades have left most people, and even many industry executives, confused about the very nature of health benefits. Today, even many intelligent consumers conflate two very different concepts, health insurance and a health services plan. The former, the first health benefit offered to employees by their companies after World War II, came generally in the form of a major medical policy that indemnified the employee for expenses above a deductible threshold. Managed care, however, was marketed as a health services plan, in which consumers paid a fixed amount and received an enhanced bundle of services, usually including routine check-ups and preventive care not covered under typical major medical plans. But employees also had to deal with restricted provider panels and more rigorous utilization review.
Employees didn't like these constraints, and they pressured employers and insurers for options, creating an alphabet soup of hybrid arrangements (PPOs, EPOs, POS plans, etc.). But most of these lack the very features that made managed care an economically attractive concept in the first place. The upshot is that today we have health insurance products masquerading as health services plans. This isn't deception on the part of insurers and employers; it is, rather, part of a broader misconception of the changes that have occurred.
Still, the consequences are profound. Many employees' costs have gone up, amplified perhaps by perceptions developed as they tried restricted-panel HMOs (with few out-of-pocket expenses) and then switched back to less restrictive products where deductibles and co-payments are significant features. Employees' experiences with (or beliefs about) managed care have created an expectation that their health benefits will come in the form of a health services plan, not insurance. They are now beginning to experience sticker shock when looking at the costs of high-choice products. This situation is analogous to expecting your car insurance policy to include coverage for washing, waxing, and oil changes, and being surprised when your premium skyrockets.
A Rational Marketplace
These differences won't go away with the onset of the defined-contribution revolution, but consumers will be able to sort through the confusion and select products that best fit their circumstances. The underwriting structure of defined-contribution retailing will, at long last, create a rational marketplace.
We envision a three-tiered risk structure as a way of thinking about purchasing decisions under defined-contribution approaches. Under this scheme, the roles of the players (employers, consumers, insurers, intermediaries) are much clearer and product arrays sort out into a more clearly understandable set of choices. Employers and consumers will need to think about the three levels of risk that generally are masked in one overall premium today:
1. Catastrophic/extraordinary coverage will, most likely, continue to be borne by employers. Stop-loss coverage is a feature virtually everyone needs, regardless of product or plan type. Given sufficient group size (about 200 is the minimum for a $50,000 stop-loss policy), coverage is fairly inexpensive — about $30 to $50 per month in most cases. Even under a defined-contribution approach, we anticipate most employers purchasing this for their employees. This is only a small amount more per month than many large employers currently spend simply to administer their health-benefits plans.
2. Normal risk products will be purchased by employees with defined-contribution dollars. Already covered for catastrophic loss, employees would enter the retail marketplace, almost certainly through an online system. An employer's contribution might be combined with that from a spouse's employer. What consumers purchase will be determined by their appetites for risk — essentially "drawing the line" on deductibles and co-pays. The more risk they assume, the smaller their premiums.
3. Out-of-pocket costs and risks borne by the employee, the final tier of the model, will drive a move toward higher deductibles. Consumers will discover that they have very limited leverage on premiums if they insist on low deductibles. For example, doubling a deductible to $500 from $250 would produce only about a 6 percent savings on premium payments, whereas increasing the deductible to $2,000 would lower the premium by about 25 percent. Such considerations are likely to reinvigorate the demand for limited-panel HMOs as a mechanism for reducing one's risk for out-of-pocket expenses.
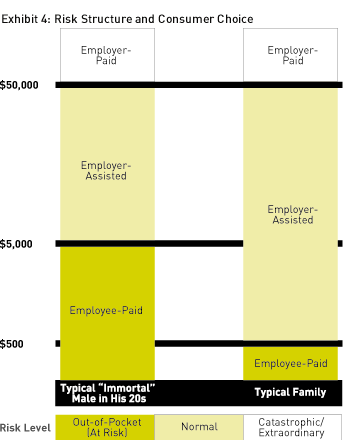
Although some of the harsh realities of cost/feature trade-offs may be exposed in the early days of the transition, the overall effect will be to clarify and simplify products, risks, choices, and costs. Two major product categories will emerge. For those who see themselves being at low risk ("immortal" single males in their 20s, for example), high-deductible, high-choice insurance products will dominate. People with families (or those starting them) will likely trade some choice for limited-panel health-services plans (e.g., HMOs). (See Exhibit 4, below.) The affluent, regardless of health status, would likely continue to pay differentials to maintain a high level of choice offered by more traditional insurance (indemnity) products.
The Medicare system, already experimenting with vouchers (an implicit defined contribution), could also fit into the defined-contribution system by allowing beneficiaries to choose between insurance and health-services plans on a community-rated basis. Working couples could combine their defined-contribution dollars and select a single, more comprehensive product. Today, without the coordination of benefits, these couples are often forced to choose between two marginal sets of coverage.
Product innovation and mass customization will also take hold as part of this more rational and consumer-driven paradigm. Once freed from offering a limited product set to a given group, insurers can design new products tailored to specific needs. For example, one could envision a low-cost insurance product that would require the customer to get routine care (age- and gender-appropriate) but pay for it out-of-pocket — the benefit of which could be not only lower premiums, but also a richer set of benefits if the policyholder does become ill ("do the required maintenance and we'll give you a full warranty on everything else").
Many other products are possible along the same lines, requiring certain "healthy" behaviors in exchange for enhanced benefits and lower costs. One can also envision health-services plans that reduce costs by relying heavily on advanced practice nurses for routine care — a difficult product to mandate for one's employees today, but one with great potential attraction in a more customized, consumer-driven market.
In an open marketplace with low penalties for switching products or plans, transparency of products and performance will foster intense competition for customers. Consequently, customer service will rise as insurers move from a wholesale to a retail mentality in their relationship with policyholders. Customer service and clinical data will be readily available to consumers through Web-based retailers of health plans.
Employers, too, will innovate, purchasing certain specific types of coverage beyond the defined contribution for their employees, based on enlightened self-interest. For example, because of cost, many consumers might select products that do not provide substance-abuse services. Some employers, on the other hand, might see this coverage as a valuable mechanism for reducing absenteeism, turnover, and accidents. Purchasing special-purpose coverage based on business needs could become common.
Consumers will also begin to make trade-offs that will moderate the seemingly limitless demand for medical services. By making explicit decisions up front about risks, features, and prices, consumers will have incentives to compare different treatment options and approaches. Should I treat that gallbladder disease by surgery or medicine, or can I make lifestyle changes? Is that branded pharmaceutical really better than the generic? Does the data show this cheaper alternative procedure to be as effective as that more expensive traditional treatment?
Dictating or mandating these choices is a hopeless and thankless effort, but empowering consumers to make these choices for themselves could be a positive force for real change. Much as reduced consumption rates under the early days of managed care permitted the addition of coverage for routine care, further real reductions in consumption rates could free up billions of dollars in economic value for enhanced benefits, reduced costs, and increased profitability for the health-care and -benefits providers.
Unfolding Opportunity
As with any new approach, it is very easy to describe the current paradigm and to envision a new one. The problem is that transitions don't occur magically from one mature concept to the next. The messiness in the middle is why change is hard — and some guidance in anticipation of that coming messiness seems in order.
Even at this early stage, the challenges and opportunities are anticipated:
- Employment-based group underwriting may survive the first wave of change. That is, a consumer would access a Web-based plan retailer (i.e., HMOsRUs.com) as a member of a specific employer or affinity group. This vestige of the old world may be necessary to avoid Darwinian underwriting that would penalize people with high-risk profiles. In the future, however, assigned risk pools, non-employment-based groupings, or other innovations could be used to ensure fairness for the individual.
- Medical savings accounts or other tax-advantaged approaches may be necessary to permit consumers to pursue risk horizons beyond a single plan year. This could, for example, permit the "immortal" single males in their 20s to fund in advance their higher risk years (e.g., parenthood, middle age) with today's excess defined contribution.
- Industry players who wait for a defined-contribution trend risk missing the wave entirely. The surf will crash over them and benefit the first movers who establish defensible long-term positions. Furthermore, those insurers who fail to prepare for a more Web-savvy and health-conscious consumer not only will fail in the world of defined contribution, but won't survive long in today's world.
- It is not too early for insurers to start strategizing to compete in the world of defined-contribution health benefits. Value chain roles (and potential niches) in product design and underwriting, distribution and sales, information aggregation, transaction processing, e-commerce infrastructure, and so on are all up for grabs.
- Defined-contribution health-benefits plans may lend momentum to the existing benefits outsourcing trend. Total benefits outsourcers seem poised for growth as companies seek ways to reduce costs and focus on their core activities. Some large insurers may even forward-integrate by acquiring (or allying with) major benefits managers or outsourcers.
- Some large insurers may attempt to catalyze the coming revolution. One way they may do so is by approaching major accounts with attractive propositions for prototype products tailored to the new defined-contribution parameters.
- E-commerce players also need to begin staking out their distinctive roles. Who will become the HMOsRUs.coms of the future — and what infrastructure challenges will these Internet players face?
- Hospital systems, physician groups, and other health-care providers may become bigger players if limited-panel HMO products regain popularity and can be locally or regionally branded. E-commerce would level the playing field for these scale-disadvantaged competitors.
Who in 1970 would have predicted that in 2000, tens of millions of Americans would be actively managing their retirement portfolios with home computers? We see an analogous transition about to happen with health benefits. Indeed, employer-managed, defined-benefit health plans will be largely gone within the next 15 to 20 years, and perhaps sooner.
Their demise seems inevitable — to winners and losers alike in the coming transition to defined-contribution, consumer-driven health benefits. ![]()
Reprint No. 00204
| Authors
J. Philip Lathrop, lathrop_phil@bah.com J. Philip Lathrop is an advisor on managed care to Booz Allen Hamilton. Gary Ahlquist, ahlquist_gary@bah.com Gary Ahlquist is a senior vice president with Booz Allen Hamilton’s Chicago office. He specializes in the strategy-driven transformation of insurance companies, health plans, and health-care providers. David G. Knott, knott_david@bah.com David G. Knott is a vice president with Booz Allen Hamilton in New York. Dr. Knott leads the firm’s strategy work in the health services sector. |

